Weight Loss After Stopping PPI
Proton pump inhibitors (PPIs) are frequently used to assist with indigestion and ulcers. While they successfully give alleviation, concerns have been raised in regard to their drawn-out use and likely effect on weight.
So, does weight loss occur after stopping PPI?
When you stop taking PPIs, some people may experience changes in their weight, but no clear evidence shows significant weight loss. However, long-term PPI use has been linked to weight gain, though individual experiences may differ.
This article examines weight changes after stopping PPIs and what factors influence this.
What Are PPIs?
Proton pump inhibitors (PPIs) are medicines that work by reducing the amount of acid your stomach makes. This helps relieve uncomfortable symptoms and helps with the healing of ulcers. PPIs target specific cells in the stomach to achieve this effect.
Uses
PPIs are commonly prescribed to manage the following conditions:
- Heartburn and Acid Reflux
- Gastroesophageal Reflux Disease (GERD)
- Stomach Ulcers
- Underlying Causes
- Inflammation in the Esophagus
Medications that are PPIs
PPIs are available in both prescription and over-the-counter (OTC) forms. Some of the commonly used PPI medications include given below in a chart:
| Prescription PPIs | OTC PPIs |
| Omeprazole (Prilosec) | Omeprazole (Prilosec OTC) |
| Esomeprazole (Nexium) | Esomeprazole (Nexium 24HR) |
| Lansoprazole (Prevacid) | Lansoprazole (Prevacid 24HR) |
| Dexlansoprazole (Dexilant) | Omeprazole/sodium bicarbonate (Zegerid) |
| Rabeprazole (Aciphex) | |
| Pantoprazole (Protonix) | |
| Omeprazole/sodium bicarbonate (Zegerid) |
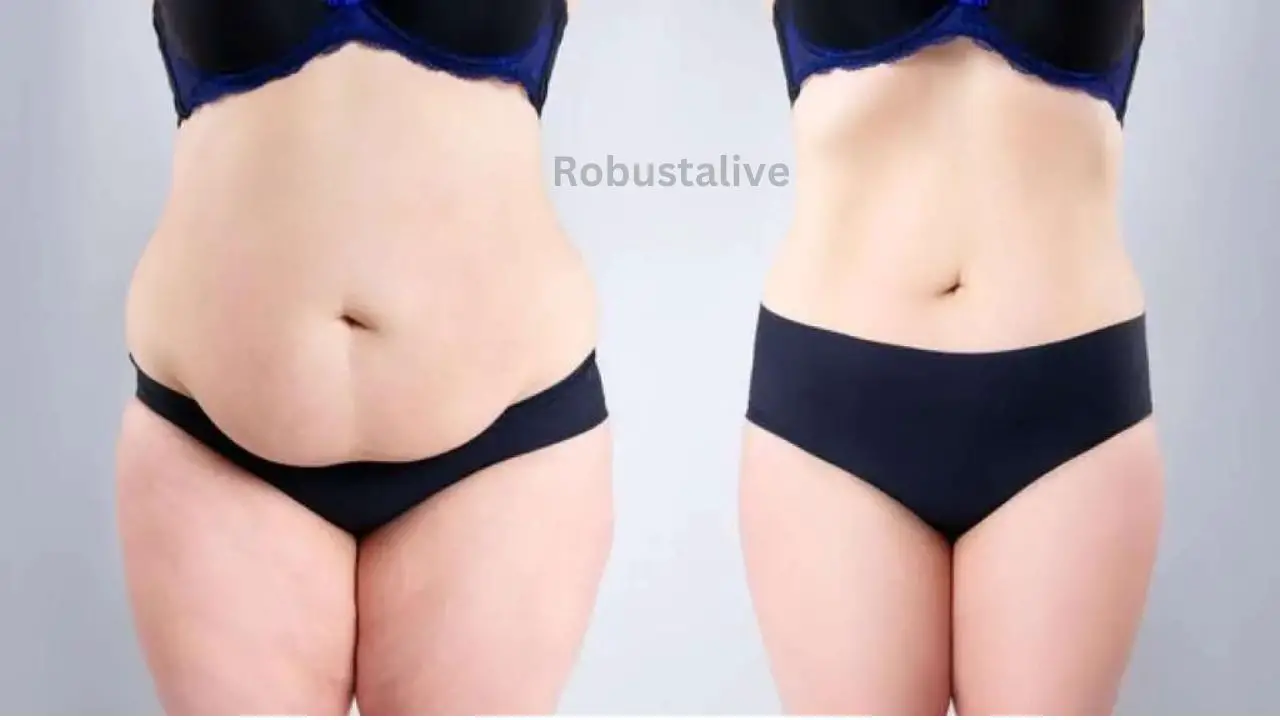
Weight Loss After Stopping PPIs
When you discontinue medicines for heartburn like proton pump inhibitors (PPIs), the effect on your weight can range from a man or woman to a person. Some people might observe changes in their weight, while others may additionally no longer experience tremendous differences. It’s critical to recognize that they have an effect on stopping PPIs that can vary for every individual.
The Link between PPIs and Weight Gain
Researchers have determined a doable connection between long-term PPI use and weight gain. For example, one located out about has determined that extended use of PPIs can lead to undesired weight gain, with an average extent of 3.5 kilograms (7.7 pounds) over about two years. This discovery has raised worries about the potential for manageable weight gain in a similar trend.
How PPIs and Heartburn Relate to Weight Gain
Many people take PPIs to manage heartburn symptoms, also known as GERD. Interestingly, weight gain can contribute to the development or worsening of GERD. Thus, using PPIs might create a cycle where weight gain leads to more heartburn, requiring continued PPI use.
PPIs can also disrupt bowel function and promote the growth of harmful gut bacteria, potentially leading to weight gain and other stomach issues.
The Possibility of Weight Loss After Stopping PPIs
You may wonder if weight loss is possible after discontinuing PPIs. While no specific scientific evidence supports significant, unexplained weight loss associated with stopping PPIs, long-term PPI use has been linked to weight gain over time.
Understanding Weight Changes and PPI Withdrawal
Individual experiences during PPI withdrawal can vary, and not everyone may experience weight loss after stopping PPIs. Individual body characteristics and withdrawal symptoms can influence weight changes during PPI withdrawal.
Factors Influencing Weight Changes
Changes in appetite can significantly determine weight gain or loss when you stop taking PPIs. Some individuals may experience diarrhea as a withdrawal symptom. This symptom can contribute to unexplained weight loss. However, it is important to note that these effects are not universal and may not occur in everyone.
Long-Term PPI Use and Weight Gain
Concerns have been raised regarding the potential weight gain associated with prolonged use of PPIs, such as omeprazole. While the exact reasons behind this connection remain unclear, it is generally advised against using PPIs for an extended period to manage acidity or ulcers due to the possible risks and side effects involved.
Remember to Consult a Healthcare Professional
If you are concerned about changes in your weight or contemplating discontinuing the use of PPIs, seeking guidance from a healthcare professional is crucial. They can provide personalized advice and support you in safely navigating this process.
Why Stop Taking PPIs?
Although PPIs effectively alleviate acid reflux symptoms, excessive or long-term usage may pose health problems. Hence, considering the discontinuation of PPIs due to potential side effects and long-term implications remains a valid consideration.
Some of the reasons to stop taking PPIs include:
Side Effects of PPIs
In most people, rare side effects can occur from taking PPIs. Here are the common side effects:
- headaches
- nausea
- diarrhea
- abdominal pain
- bloating
Health Risks
Long-term use of PPIs has been associated with:
- increased risks of kidney disease
- dementia
- bone fractures (wrist, hip, and spine)
- community-acquired pneumonia,
- Clostridium difficile,
- Campylobacter
- drug-induced lupus erythematosus
- Salmonella infections
- acute interstitial nephritis (kidney inflammation)
- low magnesium levels (hypomagnesemia)
- low vitamin B-12 levels
However, more research is required to establish definitive cause-and-effect relationships,
Overuse and Caution
Sometimes, healthcare specialists prescribe PPIs for a longer duration of time than they should, which would perhaps no longer be very safe. Using these drugs for a lengthy time can have risks, and we do not understand everything about their long-term results due to the fact there hasn’t been ample research. So, it is vital to be cautious when taking PPIs for a prolonged period.
Withdrawal Symptoms
When stopping PPIs, individuals may experience a range of withdrawal symptoms. These symptoms can vary from person to person, but some common ones include:
- Heartburn: Increased heartburn or acid reflux symptoms can result from discontinuing PPIs due to the reduction in acid suppression, causing a rebound effect.
- Stomach Pain and Nausea: PPI discontinuation may result in unpleasant stomach pain, nausea, and discomfort.
- Headaches and Dizziness: Some individuals may experience headaches and dizziness as their body adjusts to the absence of PPIs.
- Emotional and Psychological Symptoms: Sometimes, when a person stops taking PPIs, they may experience emotional and psychological symptoms. These can include anxiety, depression, and a sense of withdrawal.
These symptoms can be uncomfortable and may last several weeks or months. It is essential to talk to a healthcare professional before stopping PPIs.
How to Manage PPI Withdrawal Symptoms?
Here are some strategies to help manage PPI withdrawal symptoms:
- Gradual Reduction: Your doctor can help you develop a gradual tapering schedule to decrease your PPI dosage, allowing your body to adjust more smoothly.
- Lifestyle Modifications: Take smaller, more frequent meals – avoid spicy foods, caffeine, and alcohol, drink lots of water, get enough rest – try stress-relief activities like yoga or meditation.
- Symptom Relief: Maybe, over-the-counter antacids or even acid-reducing medications during withdrawal will give you temporary heartburn or acid reflux symptoms relief. But definitely talk to your health care professional before taking any more medicines.
How to Stop Taking PPIs?
Stopping PPIs abruptly can lead to increased acid production, known as rebound acid production, which can cause a flare-up of GERD symptoms. To discontinue PPI use effectively and minimize rebound symptoms, you can follow these three main strategies:
Gradually Taper Your PPI:
Reduce your PPI dose gradually over three weeks under the guidance of your healthcare provider.
Take PPI On-Demand:
If you’ve been using a PPI for a while, switching to “as-needed” or “on-demand” use makes sense for you.
Instead of taking the daily dose, you take the medication only when GERD symptoms bother you.
This approach may not work well if you start PPI treatment for the first time but it can go very well if you have been on PPIs for some time.
Explore Other GERD Medications:
You can consider alternative GERD medications if you experience rebound symptoms while trying to stop PPIs.
- H2 blockers are one option; they help reduce stomach acid production. Famotidine (Pepcid, Zantac) and cimetidine (Tagamet) are examples of H2 blockers.
- Antacids can also be used. They work by neutralizing stomach acid and providing quick relief. Examples include calcium carbonate (Tums) and calcium carbonate/magnesium hydroxide (Rolaids).
- Cimetidine (Tagamet) can interact with various medications, such as warfarin, phenytoin, and certain antidepressants.
Discuss these options with your healthcare provider to determine the most suitable alternative medication.
Seek Professional Guidance:
If you experience severe rebound symptoms or if they persist for more than two months after stopping PPIs, consult your healthcare provider. This could indicate a more complex GERD or another underlying issue that requires extended PPI treatment.
How To Lose Weight After Stopping PPI?
After stopping PPIs, focus on healthy habits to lose weight:
- Eat a Balanced Diet: Include fruits, vegetables, lean proteins, and whole grains in your meals. The foods give you the essential nutrients so you are fuller for longer.
- Limit Sugary and High-Calorie Foods: Reduce sugary treats and high-calorie snacks. Opt for healthier choices instead.
- Stay Active: Regularly exercise to burn calories and boost your metabolism. Even simple activities like walking or dancing can make a difference.
- Drink Plenty of Water: Drink enough water throughout the day. Water helps control appetite and supports your weight loss efforts.
- Reduce Salt Intake: Too much salt can lead to water retention and bloating. Cut down on salty foods to support your weight loss journey.
- Limit Alcohol Consumption: Alcoholic beverages pack a punch when it comes to calories, making them a potential roadblock on the path to shedding pounds. To make meaningful progress towards your weight loss goals, it is advisable to minimize or abstain.
- Get Enough Sleep: To ensure better health, it is important to prioritize getting enough sleep. Making an effort to achieve 7-9 hours of quality sleep each night can play a significant role in maintaining a healthy weight.
- Manage Stress: To effectively manage stress, individuals are encouraged to practice various relaxation techniques. One such technique involves engaging in deep breathing exercises or meditation.
Remember, losing weight takes time and patience. Focus on making small, sustainable changes to your lifestyle, and celebrate your progress along the way.
Frequently Asked Questions (FAQs)
Does Omeprazole Stop You Losing Weight?
There is no direct relationship between omeprazole and weight increase or decrease. However, if your situation gets better after taking omeprazole and your digestive signs and symptoms go away, you may find that your starvation increases, which could result in weight gain.
Does Omeprazole Make You Retain Fluid?
A study discovered that 0.45% of those utilizing omeprazole experience edema, otherwise called water maintenance. More seasoned ladies taking the medicine for under a month are bound to have this issue.
How Long Does It Take For PPIs To Work?
PPIs usually take a few days to start working and may need up to a week for full effect. For example, Protonix (pantoprazole) can reduce acid by 85% within seven days. But the exact time may vary, so it’s best to ask your pharmacist or doctor about your specific PPI.
Conclusion
To conclude, even though there is now not any stable proof that stopping PPIs causes weight reduction, long-term PPI use has been linked to weight increases. For your wellness, put an emphasis on a healthy diet, exercise, and stress reduction.